Chronic prostatitis is one of the most common diseases in mature men. Inflammation of the prostate will greatly reduce the quality of life and become the cause of psychosomatic and sexual diseases. The lack of sufficient information about the nature of this disease makes the treatment of chronic prostatitis a difficult task, requiring the patience of patients and their doctors.
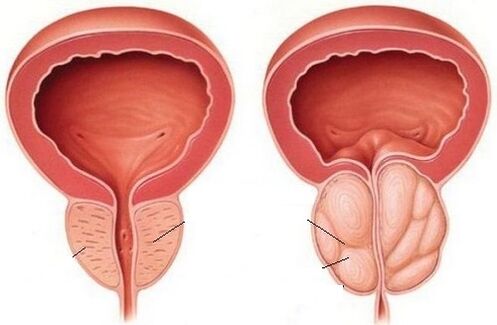
Prostatitis is an inflammatory degeneration of the prostate.
classification
The National Institutes of Health (NIH USA) has developed and proposed the following classifications of chronic prostatitis:
- Chronic bacterial prostatitis;
- Chronic non-bacterial prostatitis (with or without signs of inflammation);
- Chronic asymptomatic prostatitis.
Modern andrologists adhere to this classification in the diagnosis and treatment of prostatitis. Acute prostatitis is prominent respectively. Knowing which category the identified pathology belongs to, doctors will be able to choose the best treatment plan and achieve significant success in treating the disease.
Causes and risk factors
Divided into bacterial and non-bacterial chronic prostatitis is not accidental. The various causes of the disease determine the treatment strategy, and to a large extent affect the outcome of the disease.
Chronic bacterial prostatitis
Chronic bacterial prostatitis occurs in 10-15% of patients. The direct cause of disease development is the penetration of pathogenic and opportunistic flora into the prostate. By definition, the prostate is free of bacteria. The prostate may be infected through the urethra as well as blood and lymph. During the inspection, the following microorganisms were most commonly detected:
- Escherichia coli (up to 95%);
- amoeba;
- Klebsiella
- Pseudomonas.
Representatives of Gram-positive bacteria (Staphylococcus, Streptococcus) are very rare. In some cases, the growth of two or more microorganisms is noticed (mixed infection). May be infected with pathogenic bacteria (chlamydia, trichomoniasis, gonococcus, etc. ).
Most of the microorganisms detected during the inspection are representative of the normal flora. Under normal circumstances, they will not harm the human body and can exist peacefully on the mucous membranes of the urinary system and digestive tract. Under certain conditions, the growth and reproduction of conditional pathogenic flora occurs, which can cause inflammation of the prostate tissue and all symptoms of the disease.
Risk factors for chronic bacterial prostatitis:
- Failure to observe personal hygiene;
- Low temperature;
- Genital trauma;
- Inflammatory diseases of the urinary system;
- The existence of sexually transmitted infections.
All of these will lead to a decline in local and systemic immunity and the natural reproduction of opportunistic flora in the prostate. It is not ruled out that infection can enter the urethra through inflammatory diseases of the reproductive tract. The possibility of prostatitis increases with existing urethritis, cystitis, and colitis.
Chronic nonbacterial prostatitis
There are several theories regarding the occurrence of this disease:
- Chemical inflammation theory. . . Throwing urine into the prostate during urination can cause urate deposition and inflammation. Urethral stricture (stenosis) and other developmental abnormalities can promote prostate reflux in the urethra.
- Immunity Theory. . . This version is based on autoimmune damage to prostate tissue after exposure to bacterial antigens. Consider the genetic susceptibility of this pathological form.
- Neurogenic theory. . . Violating the innervation of the pelvic region can cause stagnation of blood in the organs and lead to the development of prostatitis.
In the development of non-bacterial prostatitis, the following risk factors should also be paid special attention:
- Sedentary work;
- A sedentary lifestyle;
- bad habits;
- Stress and emotional overload;
- Long-term abstinence.
These risk factors stimulate the development of prostate congestion, leading to violations of the microcirculation of the pelvic organs. Microbial factors only play a role in the initial stages of disease development. In the future, its importance will decrease, and autoimmune processes and nutritional disorders in the prostate tissue will appear.
According to statistics, 85-90% of men suffer from non-bacterial chronic prostatitis (not directly related to pathogenic or opportunistic bacterial infections).
symptom
Chronic prostatitis mainly occurs in men aged 25-40. With age, the likelihood of suffering from this disease increases. In old age, inflammation of the prostate is usually combined with adenoma-benign tumors of the prostate.
Signs of chronic prostatitis:
- Faint pain in lower abdomen;
- Radiation to groin, scrotum, perineum, lower back, bone pain;
- Increase discomfort during sexual intercourse and bowel movements.
Urination disorders are typical:
- Frequent urination;
- A small part of urine is excreted;
- Feeling of incomplete bladder emptying;
- The appearance or intensification of pain when urinating;
- The urine flow is slow and intermittent.
The latter symptom is characteristic of prostate adenomas and usually occurs in the context of chronic prostatitis.
With the long-term development of diseases, diseases will appear in the sexual field:
- Decreased libido;
- Worsening erection;
- Reduce the time of sexual intercourse;
- Premature ejaculation
- Pain in the lower abdomen after ejaculation;
- Lack of spontaneous morning erections.
Chronic prostatitis is one of the main causes of erectile dysfunction, in which men cannot achieve and maintain an erection sufficient for sexual intercourse. This condition can seriously interfere with the life process and may lead to depression and other psychological and emotional disorders.
The occurrence of chronic asymptomatic prostatitis does not have any clinical manifestations. The urologist accidentally discovered this disease during the examination. Although there are no symptoms, inflammation of the prostate can cause serious complications, erectile dysfunction and other health problems.
complication
Emitted prostatitis provokes the development of the following conditions:
- Prostate abscess;
- Cystitis and pyelonephritis (inflammation of the bladder and kidneys);
- Vesicle inflammation (seminal vesicle inflammation);
- Erectile dysfunction;
- Infertility.
The sooner a disease is detected and treatment is started, the better the chance of a good result for the disease.
Diagnostic procedure
The following methods can be used to detect chronic prostatitis:
Urologist check
In private appointments, doctors focus on the complaints of patients. Examine the external genitalia and perform a digital rectal examination of the prostate. During palpation, the doctor will assess the size and shape of the glands. In the case of chronic prostatitis, the organs will be slightly larger. This procedure is combined with the collection of prostate secretions for microbiological examination.
Four cup samples
The main method that allows you to identify the inflammatory process in the prostate and distinguish it from other diseases. The collection of materials is carried out in several stages. In the morning, 5-6 hours after leaving the toilet, a man urinates in two jars-the first part (initial) and the second part (middle) of urine. In the first part, the contents of the urethra are washed away, and in the second part, the bladder is washed away. The third part of urine is collected after prostate massage, allowing you to assess the condition of the prostate. Collect the secrets of the prostate separately for bacterial culture.
In urinalysis, two parameters are evaluated: the number of white blood cells and red blood cells. With prostate disease, the white blood cell count in the third part of the urine increases. Generally, their number does not exceed 10 in the field of view.
Microbiological examination
When performing a three-cup test, not only the number of white blood cells must be evaluated, but also materials must be taken for bacterial inoculation. If you suspect chronic prostatitis, the doctor is particularly interested in the third part of the urine. Based on the results of the examination, the doctor can determine the cause of the disease and choose the best antibiotic treatment.
The identification of opportunistic bacteria with a titer greater than 10 has diagnostic value.3Detection of CFU/ml or any number of clear pathogenic microorganisms.
Bacteriological culture of prostate secretions
Bacteriological seeding of prostatic fluid makes it possible to assess the nature of the process (with or without infection) and to determine the type of pathogen.
During prostate massage, the doctor needs to perform a bacteriological examination of the secretions before taking the third part of urine. The results obtained can also determine diagnosis and treatment strategies.
Diagnostic criteria of chronic bacterial prostatitis:
- Detection of opportunistic microorganisms in the third part of urine or prostate secretion with a titer higher than 103CFU/ml.
- The number of opportunistic bacteria detected in the third part of urine or prostate secretion is significantly higher (10 times) than the number of bacteria in the second part of urine.
- Identify pathogenic microorganisms in the third part of urine or prostate secretions.
Ultrasound
Ultrasonography allows you to assess the size of organs and determine the accompanying pathology. Usually, chronic prostatitis is associated with prostate adenoma-benign tumor.
Treatment principles
The goal of treatment of chronic prostatitis is to eliminate the inflammatory process, activate blood flow and improve organ nutrition. When pathogenic or opportunistic microorganisms are detected at high titers, they will be eliminated. Pay special attention to correcting the lifestyle and stimulating the body's defenses.
medical treatement
The following drugs can be used to treat chronic prostatitis:
- When choosing antibacterial drugs, consider the identified pathogens.
- Anti-inflammatory drugs can reduce inflammation and relieve pain.
- Means to promote urination (α-blockers, which relax the muscles of the urethra and stimulate the flow of urine).
- Means to increase blood flow to the pelvic organs.
The choice of antibiotic will depend on the pathogen identified. When choosing a drug, its ability to penetrate the blood prostate barrier and accumulate in the prostate tissue should be considered. These conditions can be met by fluoroquinolones. Macrolides and tetracyclines can also be used to treat chronic prostatitis.
According to the recommendations of the European Association of Urology, the course of antibacterial treatment should be at least 2 weeks after the initial diagnosis is established.
After receiving the bacteriological research results and confirming the bacterial nature of the disease, the treatment can last for 4-6 weeks. This method can not only eliminate the pathogen of the disease, but also prevent the recurrence of prostatitis.
Unfortunately, antibiotic treatment is not always effective. For a long time, many microorganisms successfully existed in the secret of the prostate and acquired resistance to antibiotics. Bacteria form special biofilms and form microbial colonies covered with complex polysaccharide structures. Most antibacterial drugs cannot penetrate this biological barrier, which greatly reduces the effectiveness of the treatment. This problem can be avoided by using modern antibiotics. Not only can modern antibiotics penetrate and heat the prostate tissue, but they can also pass through the biofilm and infect such strictly protected bacteria.
Non-drug therapy
In non-drug treatment, special attention should be paid to prostate massage. This procedure stimulates the blood supply to the prostate, eliminates congestion, and promotes the excretion of secretions. The combination of massage and long-term use of antibacterial drugs is the main method to relieve the uncomfortable symptoms of chronic prostatitis in men.
The affected physical therapy methods are used together with the action of drugs to treat chronic prostatitis. Good results can be seen by using ultrasound, laser beams, radio waves and electromyography stimulation. The shock wave massage (UHM) of the prostate is very popular. Erectile dysfunction is one of the complications of prostatitis, especially physical therapy.
Special attention should be paid to diet in the treatment of prostatitis. The following foods should be excluded from the diet:
- alcohol;
- spicy food;
- Fried and high-fat foods (including high-fat meat and fish).
The daily salt limit is 5 grams. Priority is given to fresh vegetables and fruits, herbs. It is recommended to steam.
Diet can speed up recovery, strengthen immunity, and help the body cope with the stress caused by antibiotics while curing diseases.
National Science
When symptoms of prostatitis appear, not everyone sees a doctor. Generally, men tend to use folk methods, use knowledge bases from numerous forums, and rely on suggestions from friends, relatives, and neighbors. Ignoring one's health, refusing reasonable antibiotic treatment and other traditional contact methods may threaten the development of complications and the deterioration of the overall condition. Failure to cure prostatitis in time can lead to erectile dysfunction. If you can go to the doctor on time and solve the problem with minimal loss, is it worth the risk?
Of course, in traditional medical methods, some aspects deserve special attention. Modern urology recognizes the efficacy of many herbs in the treatment of chronic prostatitis. Experts recommend herbal preparations based on the following ingredients:
- Pumpkin seed oil
- Holly
- Garden parsley
- St. John's Wort's Hypericum perforatum;
- Canadian Compositae
- Licorice root;
- Echinacea.
These ingredients can stimulate blood flow in the pelvic organs alone or in combination, eliminate congestion and stimulate the immune system.
Phytoremediation will not remove pathogenic bacteria from the body, but will help eliminate the symptoms of the disease.
Combining antibacterial drugs and prostate massage, herbal medicine can significantly improve the overall condition and speed up recovery.
prevention
The following suggestions will help reduce the risk of chronic prostatitis:
- Hypothermia of the entire body and genitals, pelvis and lower limbs is not allowed. In the cold season, it is worth wearing thermal underwear.
- The rules of privacy and hygiene must be followed, and condoms must be used to prevent sexually transmitted infections. The best way to prevent infection is to refuse casual sex.
- You should pay attention to your health and treat any diseases in the genital area promptly.
- Eating (giving up spicy, fried, and high-fat foods) and maintaining good health (sports, fitness, and walking) are not superfluous.
It is recommended that all men over the age of 30 have a regular check-up by a urologist (at least once a year). If you experience any uncomfortable symptoms, you should see a doctor as soon as possible.
FAQ
Can chronic prostatitis be cured?
Contrary to popular belief, chronic prostatitis can be successfully treated. If you follow all the doctor’s recommendations, you can eliminate the uncomfortable symptoms of prostatitis and significantly improve the quality of life.
Can chronic prostatitis be asymptomatic?
Yes, this disease can only be found after an examination by a urologist.
Is chronic prostatitis in a partner dangerous for women?
Sexually transmitted infections are usually the cause of chronic prostatitis. If the causative agent is identified, both parties must receive treatment. Otherwise, there is a risk of infection, and the effectiveness of the treatment is reduced due to the recurrence of the disease.
Is it possible to have sex with chronic prostatitis?
Yes, if the general situation allows and there are no problems in the sexual area (erectile dysfunction).
Can a child with chronic prostatitis be pregnant?
Yes, if the function of the prostate is preserved and its secrets are fully developed. It is recommended that you accept the examination and treatment of a urologist before you become pregnant. The infection that leads to the development of prostatitis is easily spread to women. Intrauterine infection of the fetus can lead to developmental abnormalities and termination of pregnancy.
How does chronic prostatitis affect the efficacy of the drug?
Chronic inflammation of the prostate threatens the development of erectile dysfunction. Due to this pathology, libido decreases, the frequency and intensity of erections decreases, and orgasm becomes painful. In the late stage, sexual activity is not possible.
Can chronic prostatitis be cured without antibiotics?
Antibiotic treatment is considered to be one of the key methods for the treatment of chronic prostatitis. In most cases, this disease cannot be dealt with without antibiotics.
Can chronic prostatitis be cured with folk remedies?
It is not feasible to get rid of chronic prostatitis with traditional medicine alone. In order to achieve the best results, complex treatments are performed using antibiotics, herbal preparations, anti-inflammatory drugs and physiotherapy methods.



























